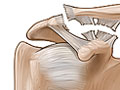
Shoulder Separation
Condition Basics
What is a shoulder separation?
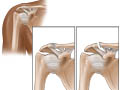
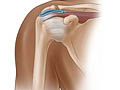
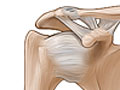
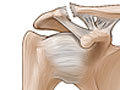
A shoulder separation is the partial or complete separation of two parts of the shoulder. It occurs when the outer end of the collarbone (clavicle) separates from the end (acromion) of the shoulder blade because of torn ligaments.
This injury occurs most often from a blow to the top of the shoulder or a fall onto the shoulder. A shoulder separation is classified according to how severely these ligaments are injured:
- In a type I injury, the acromioclavicular (AC) ligament is partially torn, but the coracoclavicular (CC) ligament is not injured.
- In a type II injury, the AC ligament is completely torn, and the CC ligament is either not injured or partially torn. The collarbone is partially separated from the acromion.
- In a type III injury, both the AC and CC ligaments are completely torn. The collarbone and the acromion are completely separated.
There are three further classifications, types IV through VI, which are uncommon.
What causes it?
A direct blow to the top of the shoulder or a fall onto the shoulder, such as a fall from a bicycle, can cause a shoulder separation.
What are the symptoms?
Symptoms of a shoulder separation include pain when the injury occurs. Limited shoulder movement as well as swelling and bruising may follow. The small joint over the shoulder may be tender. A deformity is possible at the outer end of the collarbone. There may be a bump on top of the shoulder.
How is it diagnosed?
A shoulder separation is diagnosed through a medical history, a physical exam, and an X-ray.
Your doctor will check:
- For a deformity or bump.
- The range of motion of your shoulder and other joints.
- Blood flow, by taking your pulse and assessing your skin color and temperature.
- For damage to your nerves or blood vessels.
- The muscle strength of your shoulder and arm.
- For broken shoulder bones or damage to the tendons in the shoulder (rotator cuff tear).
Your doctor will probably X-ray your injured shoulder and possibly your uninjured shoulder to help diagnose the severity of the separation.
How is a shoulder separation treated?
Treatment of a shoulder separation depends on its severity. For a type I or II injury, you support your shoulder with a sling. You typically need the sling until the discomfort decreases (a few days to a week). Early physical therapy to strengthen your shoulder and regain range of motion is important for recovery and to prevent frozen shoulder (adhesive capsulitis), a condition that limits shoulder motion . You can return to normal exercises and activities as your pain and other symptoms go away.
Treatment for type III injuries can vary. Some doctors treat them with a sling and physical therapy, while others feel surgery may be needed.
Type IV through VI injuries should be evaluated for possible surgery.
Related Information
Credits
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: July 31, 2024
Author: Ignite Healthwise, LLC Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.