St. Luke’s Newsroom
When people thrive, communities grow stronger. Explore stories highlighting how St. Luke’s supports our patients, neighbors and communities, collaborates with nonprofit organizations to improve health, and celebrates team members, partnerships and milestones.
Featured Articles
News & Announcements
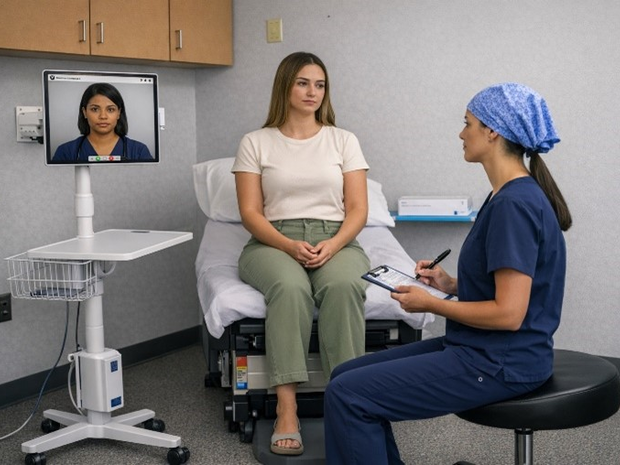
St. Luke’s and Penn State partner to expand compassionate, 24/7 sexual assault care through telehealthThis collaboration ensures patients at St. Luke’s can receive expert sexual assault forensic exams 24 hours a day, seven days a week.

News & Announcements
In the air or office, St. Luke’s employee brings passion to vastly different rolesSt. Luke’s Employee works as both an instructional designer and pilot for St. Luke’s.

News & Announcements
‘I’m still here’: St. Luke’s data engineer finds new voice while fighting ALSSuch a simple sentence, but it says so much. And the ability for others to hear it, that means everything to Ward.

Community Health & Engagement
Finding community in a new way, St. Luke’s Magic Valley patient gives back to ‘amazing place’A few miles into the serene Sawtooth Mountains, Joyce Gordon was in the final stretches of a long bike ride on a warm winter day. One small patch of ice would change that.
Read more News & Announcements from St. Luke’s
View all
News & Announcements
St. Luke’s teams up for Idaho Jobs Explained video series showcasing health care careersSt. Luke’s recently teamed up with Idaho LAUNCH and Idaho Public Television to create Idaho Jobs Explained, a brief and engaging video series that highlights in-demand careers across Idaho.

News & Announcements
St. Luke’s and Penn State partner to expand compassionate, 24/7 sexual assault care through telehealthThis collaboration ensures patients at St. Luke’s can receive expert sexual assault forensic exams 24 hours a day, seven days a week.

News & Announcements
In the air or office, St. Luke’s employee brings passion to vastly different rolesSt. Luke’s Employee works as both an instructional designer and pilot for St. Luke’s.

News & Announcements
‘I’m still here’: St. Luke’s data engineer finds new voice while fighting ALSSuch a simple sentence, but it says so much. And the ability for others to hear it, that means everything to Ward.

Community Health & Engagement
Finding community in a new way, St. Luke’s Magic Valley patient gives back to ‘amazing place’A few miles into the serene Sawtooth Mountains, Joyce Gordon was in the final stretches of a long bike ride on a warm winter day. One small patch of ice would change that.
Read more News & Announcements from St. Luke’s
View allAdvancing Community Health

Community Health & Engagement Finding community in a new way, St. Luke’s Magic Valley patient gives back to ‘amazing place’
A few miles into the serene Sawtooth Mountains, Joyce Gordon was in the final stretches of a long bike ride on a warm winter day. One small patch of ice would change that.

Community Health & Engagement Air St. Luke’s partners with Colorado team for avalanche rescue training in Wood River Valley
Helicopters, dogs and some out-of-state compatriots were on hand for a multi-day specialized avalanche search and rescue training school.

Community Health & Engagement Connecting care: How St. Luke’s teams are using focused data to address major Idaho issue
Though Idaho has one of the lowest rates of breast cancer screenings in the nation, St. Luke’s teams are utilizing data to identify areas of greatest need in our communities.

Community Health & Engagement All in the family: Mom, son, daughter team up to serve patients in St. Luke’s Elmore operating rooms
It is one thing to have a work environment that would be described as a “family atmosphere.” In the operating rooms at St. Luke’s Elmore, it is literal.

PATIENT STORIES
While enduring multiple surgeries and intensive treatments for two bouts of cancer at St. Luke’s Children’s, Maddie’s determination never wavered. Now in recovery and continuing follow up care, she looks ahead with resilience.
St. Luke’s 2026 Children’s Miracle Network Champion, Maddie




