Dr. Pate’s Prescription for Change
Co-Management Model Benefits Patients at Risk for Hip Fracture

Better outcomes at a lower total cost of care. That’s St. Luke’s Health System’s population health goal.
And our work around hip fracture is a great example of how a multidisciplinary team has come together to improve outcomes and lower the total cost of care when it comes to patients associated with a high mortality rate and a costly course of medical care for those who survive.
Here is St. Luke’s Communications Coordinator Chereen Langrill to tell you how caregivers at St. Luke’s have teamed up to address this costly and deadly condition.
- David C. Pate, M.D., J.D.
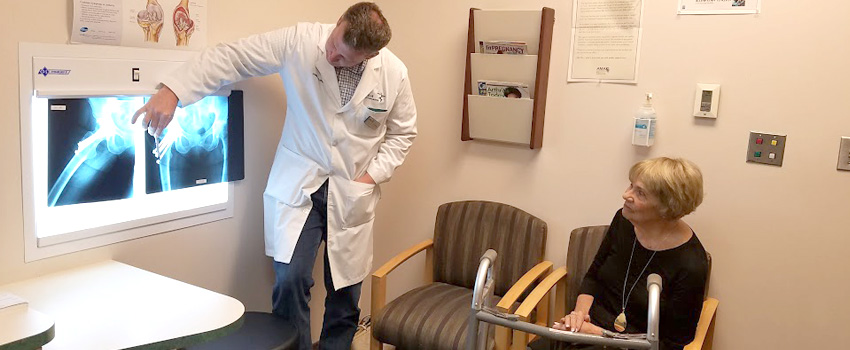
When a fall causes a hip fracture, the consequences can be devastating, particularly for older adults.
A broken hip can bring with it a long, costly recovery, and statistics show that half of patients admitted to the emergency department for a hip fracture will lose the level of activity they enjoyed prior to the injury.
To improve survival rates and recovery, a team at St. Luke’s has developed a program dedicated to improving those odds and helping patients get on their feet sooner, with fewer complications and a lower risk of further fractures.
The program is aimed at older adults at risk for dementia, anemia and osteoporosis. Within that fragile population, a simple ground-level fall can cause a hip fracture, and their weakened conditions place them at additional risk for serious complications while they are in the hospital for treatment.
Hip fractures for older adults can be life-changing. Many patients never regain the independence they had before the fracture. Some develop complications such as delirium or aspiration pneumonia. The one-year mortality for hip fracture patients is between 14 percent and 36 percent. Hip fractures are also among the most expensive diagnoses for Medicare.
“This is such a high-risk patient population,” said Dr. Britton Wells, director of St. Luke’s Hip Fracture Program. “We really need to do everything in our power to minimize complications and maximize their success rate after surgery.”
The program, which began in October 2016, targets elderly people who are most at risk for a hip fracture. It is in place in the Treasure Valley, and the team hopes to expand.
Following clinical practice guidelines from the American Academy of Orthopaedic Surgeons (AAOS), the team developed a standardized care map to streamline care and account for:
- Faster transitions from the emergency department to the operating room;
- Delivery of a fascia iliaca pain block prior to surgery;
- Appropriate use criteria from the AAOS to determine the procedural surgical approach; and
- Osteoporosis management post-discharge in collaboration with the SLHS Osteoporosis and Bone Health Program.
Osteoporosis is a common condition that can cause fractures. Known as a “silent disease” because it doesn’t have any warning symptoms, osteoporosis causes bones to weaken and makes them more likely to break in the event of a fall. An estimated 75 percent of people who fall and fracture a hip are unaware they have osteoporosis.
Education, prevention and collaboration
Patients with undiagnosed osteoporosis can be intercepted if they connect with a care provider who recognizes they are at risk. Since patients may receive care from a wide variety of providers, the team working on the hip fracture challenge has partnered with SLHS Osteoporosis and Bone Health colleagues to identify and engage these at-risk patients. The Osteoporosis and Bone Health Program is comprised of stakeholders from rheumatology, endocrinology, orthopedic surgery, radiology, physical therapy and many other areas of specialty.
Nurse Navigator Becca Humphreys is the Osteoporosis and Bone Health Program manager and coordinates post-fracture care for these patients. She generates reports identifying patients who could potentially benefit from osteoporosis education and treatment, such as those recently treated for hip fracture, and then works with primary care providers and the Bone Health care team to coordinate osteoporosis follow-up.
Those primary care providers are an important component to the program’s success, because they are often the patient’s main point of contact.
“It is surprising to me, the number of older adults who have never talked with their PCP about osteoporosis,” Humphreys said.
National research shows that 50 percent of hip fractures are preventable, and statistics also show that once someone fractures a hip, they are more likely to have another hip fracture in the future. To get in front of this challenge, the team wants to recruit support at multiple points of care to foster prevention through education. Tools provided through the cooperative programs can connect patients with the resources they need, resources that might include fall prevention education, nutrition counseling and supplements such as calcium and Vitamin D.
Providers also educate patients about the importance of taking osteoporosis treatment as prescribed. Patients sometimes stop taking osteoporosis medication because they have heard about possible side effects or because they don’t have any symptoms and think the medication is unnecessary.
“Our goal in the prevention component of this program is to provide the primary care providers – the frontline providers – with the tools to manage their patients’ bone health. We are here as a resource,” said Dr. James Loveless, who serves as St. Luke’s medical director for the Osteoporosis and Bone Health Program.

Reducing opioid use
An additional component of the program is the effort to reduce opioid use. Before the program was in place, opioids were used to control the pain patients would experience after a fracture and while they waited for an operation.
Because high doses of opioids can cause delirium, St. Luke’s is focused on fascia iliaca blocks for patients as soon as possible after they arrive at the emergency department. The local anesthetic nerve block reduces delirium rates and improves patients’ overall comfort. The goal is for the patient to receive the pain block within four hours of orthopedic consultation or being admitted from another institution.
While Kaye Naeve doesn’t represent the program’s typical patient population – she is an active, healthy older adult – she benefited from the program’s new protocol when she needed treatment for her hip fracture.
Naeve was rushing to answer her phone when she tripped and fell at her home in late October. Her family rushed her to St. Luke’s Boise and by the next day, she’d had surgery to repair the right femoral neck fracture.
As a former nurse, Naeve was grateful her care team used the fascia iliaca block instead of opioids to control pain. Naeve said that seniors metabolize opioids differently than younger adults do, making them more susceptible to delirium.
When delirium occurs, it makes patients feel disoriented and afraid.
“I’ve been so impressed with this process,” Naeve said.
Increased awareness
The concepts – and the St. Luke’s programs – have been gaining national attention. An article published in the New England Journal of Medicine this past November talked about the value of osteoporosis co-management in highly functioning hip fracture programs.
In September, St. Luke’s Boise and Meridian were recognized by the American Orthopaedic Association as a Star Performer, representing a 75 percent compliance rate with at least five out of 10 quality measures. St. Luke’s was among 75 institutions recognized by the association and was listed in the U.S. News & World Report “Best Hospitals” Guide in January.
St. Luke’s was also awarded a Joint Commission Center of Excellence certification for hip fracture management on Nov. 1, 2017. And in early January, an article written by the team was published in AAOS Now, a peer-reviewed journal published by the AAOS.
Implementing a hip fracture program makes good sense, according to Dr. Loveless, because studies show that education and prevention keep people healthier and out of the hospital.
“This problem is relatively easy to address and effective when patients work with their care team on prevention and treatment measures,” Dr. Loveless said. “The positive results for our community will be substantial.”
About The Author

Chereen Langrill was formerly a communications coordinator for St. Luke’s Health System.




