Dr. Pate’s Prescription for Change
St. Luke’s Nurse Navigators Improve Care Journey for Patients


The physicians, nurses and all members of the St. Luke’s team are very mindful that patients with significant illnesses and complicated care face significant challenges that extend beyond care moments. There may be emotional, physical and/or financial needs, for example.
It’s why we increasingly look to our nurse navigators to support and guide these patients through their care and treatment. Here is St. Luke’s Communications Coordinator Chereen Langrill, reporting on how St. Luke’s is tapping into nurse navigators and some of the many ways they are helping patients.
- David C. Pate, M.D., J.D.
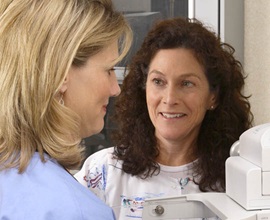
Melinda Bristol was still reeling from the news that she had breast cancer when she received a phone call from Jill Winschell, a nurse navigator from St. Luke’s Mountain States Tumor Institute in Boise.
In Bristol’s words, she was “like a deer in the headlights” following the diagnosis. She was filled with questions and anxiety, and felt isolated and scared.
After speaking with Winschell, who called within a day of Bristol’s diagnosis, she felt calm and confident about the road ahead. Winschell talked to Bristol using non-clinical words that she understood, and listened calmly as Bristol shared her fears and asked questions.
“The fact that she was there and available was huge to me because I felt so alone,” she said. “The not knowing was the scariest part for me. I didn’t even feel a need to talk with anyone else about it, because she took the fear away from me.”
Winschell is one of four nurse navigators with St. Luke’s Breast Care Services. They guide patients through every step of the medical journey, provide education and help patients remove barriers, whether financial, physical or emotional, by connecting them with the appropriate resources. They also ensure the patient’s care team is aware of the patient’s goals and concerns, ensuring all care providers are aligned with a treatment plan that best fits the patient’s needs.
For Bristol, this meant getting answers to all of the questions she had about what to expect during treatment for a tumor in the center of her left breast. A biopsy confirmed it was invasive ductal carcinoma and ductal carcinoma in situ, and her treatment plan focused on the invasive ductal carcinoma and included a lumpectomy and six weeks of radiation. She finished her radiation in December and will take an anti-hormone drug for the next five years.
Winschell guided her through diagnosis, surgery, oncology visits and radiation treatment. She contacted Bristol throughout the process, and anticipated Bristol’s needs before she could even articulate them.
“She could see in myChart when I had things coming up. She would check on me based on that information,” Bristol said. “She just seemed to always be ahead of me.”
Winschell has worked at St. Luke’s for 32 years and became a nurse navigator for Breast Care Services in 2006.
“This speaks to my heart and soul,” she said. “I can give them peace of mind, solve whatever barriers they have and educate them so they know what they’re walking into.”
The connection Winschell has with her patients lingers long after treatment ends. She was once approached in a grocery store when a grateful patient recognized her voice.
Bristol said she will forever be grateful for the support she received during such a difficult time in her life.
“I’m somebody that likes to see the big picture,” she said. “I want to know what’s going to happen and then I deal with my feelings about it.
“Talking to somebody who has dealt with so many people who have gone through the same thing was huge. Every time she talked to me about what to expect, she was right. She was right on.”
Nurse navigators serve patients throughout St. Luke’s Health System in a variety of care settings and circumstances. They play a crucial role in population health because they help patients with disease management, which can lead to better health.
Here are a few examples of how nurse navigators support patients at St. Luke’s:

Bone Health
Since joining St. Luke’s in 2004, Becca Humphreys has served in a variety of roles, including as a bedside nurse, a unit-based educator, a charge nurse and a program developer. In her newest role, as the fracture liaison nurse navigator (a component of the Osteoporosis Bone Health Program), Humphreys works closely with patients who have experienced fractures and are at risk for osteoporosis.
Her first point of contact with a patient is often when they are in the emergency department receiving treatment after a fall that caused a bone fracture. Patients who have osteoporosis often don’t know they have the disease until a fracture occurs. Humphreys can help them learn strategies to help them avoid future fractures and a loss of independence.
“This program really is about population health and using a pivotal point in a patient’s life to make a change in their trajectory,” Humphreys said.
She collaborates with ambulatory and hospital-based primary care providers, nurse practitioners and physician assistants to ensure patients receive education and intervention, regardless of how they access care. Working with specialists is key, because osteoporosis is a disease process that is managed by multiple specialties, which creates the opportunity to continue to be a guide for patients through evaluation and treatment.
“The nurse navigator is the catalyst; the glue,” said Dr. Jim Loveless, St. Luke’s medical director for the Osteoporosis and Bone Health Program.

High-Risk Pregnancies
Cindy Koster began working in St. Luke’s antepartum and labor and delivery unit in the 1990s, then moved to maternal and fetal medicine. In 2015, she developed the nurse navigator program for high-risk pregnancies because she saw the need for additional patient support.
A high-risk pregnancy means that the baby could need specialized care after the birth. When a high-risk pregnancy has been identified, Koster can help parents get the resources they will need throughout the pregnancy and after the birth. Throughout her career, Koster had worked with women who needed those extra resources and weren’t always sure which steps to take first.
“It was based on years of working in this area and knowing where the gaps were,” Koster said.
Her work focuses on fetal abnormalities and anomalies. If a newborn baby will require surgery, Koster connects the parents with the surgeon and ensures they have a care plan in place before the baby is born. In some situations, parents know their baby won’t survive. In those situations, she develops a comfort care birth plan, working closely with the parents to ensure that their wishes are met.
“We honor that baby and that pregnancy,” Koster said.
The approach has changed dramatically in the past 20 years, from a time when people were encouraged to keep their grief to themselves and move past it as quickly as possible. Now Koster makes sure families can be as involved as they want to be in the process. This can include giving them a recording of the baby’s heartbeat or encouraging the mother to enjoy her pregnancy and bond with her baby.
Some babies stay in the hospital for months. Others never get to leave. Regardless of the outcome, Koster’s goal is the same.
“For everyone, I just want to make them a little more comfortable with what’s going to happen,” she said.
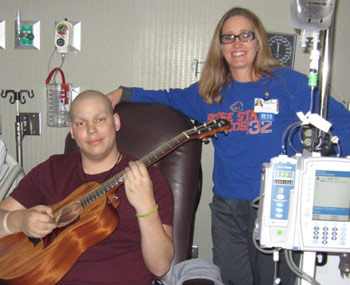
Adolescents and Young Adults
People between the ages of 15 and 39 are experiencing significant life milestones. They are teenagers just gaining independence, getting a driver’s license and transitioning to college. As young adults, they are developing their careers, getting married and having children. A cancer diagnosis creates chaos, at a time when their lives are just beginning to take off.
Darcy Gleave is there to help them keep moving forward. Gleave works as the adolescent young adult nurse navigator for MSTI. She is in a newly expanded role that began with a younger population (ages 13 to 18). The age range shifted based on a recent needs assessment conducted with the adolescent and young adult (AYA) population and MSTI staff; it also aligns with the nationally-defined AYA oncology age range.
It’s a unique position within MSTI because most other navigator roles are based on patients’ health conditions. This role is connected to a specific age group. Gleave, who also worked within inpatient pediatrics and outpatient adults at MSTI, saw this as an opportunity to help a unique patient population.
“They have jobs. They have kids. These patients are living their lives. What we need to do is help them continue living their lives and get cancer care,” Gleave said.
Many of Gleave’s patients aren’t aware of the supportive services available. Some don’t have primary care physicians. Gleave helps her patients get access to the help they need and reduce barriers that they may face. And because this patient population is experiencing many different life events, the types of services they need can widely vary.
For example, she connected a student athlete with the YMCA’s LIVESTRONG program so he could return to training once his treatment ended. Other patients are concerned about fertility after treatment.
“Once I find out what their goal is, I can help them navigate through their cancer journey,” she said.
About The Author

Chereen Langrill was formerly a communications coordinator for St. Luke’s Health System.