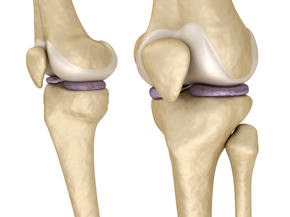
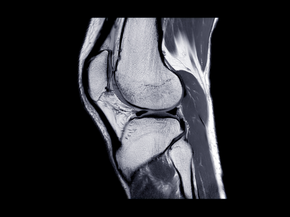
Cartilage Preservation and Restoration

Cartilage Preservation and Restoration
Preserving Mobility with Advanced Cartilage Treatments
The St. Luke’s cartilage preservation and restoration program is dedicated to the treatment of patients with symptomatic cartilage damage, including isolated cartilage defects, meniscal injuries and early arthritis. Our expert physicians will evaluate and recommend treatment options to match the physical demands of each patient’s lifestyle.
Our philosophy is to repair the cartilage damage by treating the whole patient and determining the underlying causes of damage, which can include malalignment, ligament instability and loss of meniscal function. We’ll also educate patients on the safest and latest treatment options to help them to make the most informed decision regarding their cartilage damage. Conservative, or nonsurgical, management is usually attempted before more invasive, surgical options are considered.
Our patients also have access to local and national cartilage repair and restoration research projects through partnerships with St. Luke’s Applied Research and Boise State University.
For more information on our cartilage preservation and restoration program, please call (208) 706-9118.

Our goal is to help you move freely and live fully so you can get back to doing what you love at home, at work, or at play.
Non-Surgical Approaches to Cartilage Repair and Preservation

Lifestyle Changes
Avoid aggravating activities, brace your joints for comfort, or begin physical therapy to improve strength and motion.
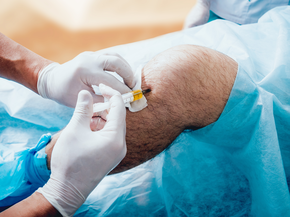
Therapeutic Joint Injections
Used to help with pain and limited motion, corticosteroid or visco supplement injections can provide relief and improved joint function.
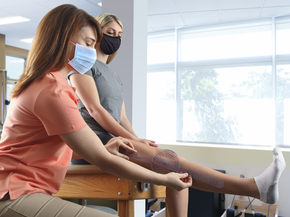
Physical Therapy
Our physical therapists can help you gain strength, increase range of motion, and restore mobility.

Platelet-Rich Plasma
This therapy involves injecting your own platelet-rich plasma into an arthritic joint or injured tendon.