
Tests to Monitor CF Patient Health
We follow CF Foundation guidelines recommending quarterly visits and annual lab tests for all patients with cystic fibrosis.

Tests to Monitor CF Patient Health
We follow CF Foundation guidelines recommending quarterly visits and annual lab tests for all patients with cystic fibrosis.
Why Are Monitoring Tests Important?
We use these tests to:
- Rule out infection
- Assess iron level
- Check for CF liver disease
- Make sure fat-soluble vitamin levels are adequate
- Check nutritional status
- Make sure bleeding times are appropriate
- Check for CF-related diabetes
- Check blood hemoglobin A1C and urine microalbumin to help patients with CF-related diabetes avoid diabetes complications
- Check bone density, sleep patterns, hearing and eyesight, as needed
Types of Testing
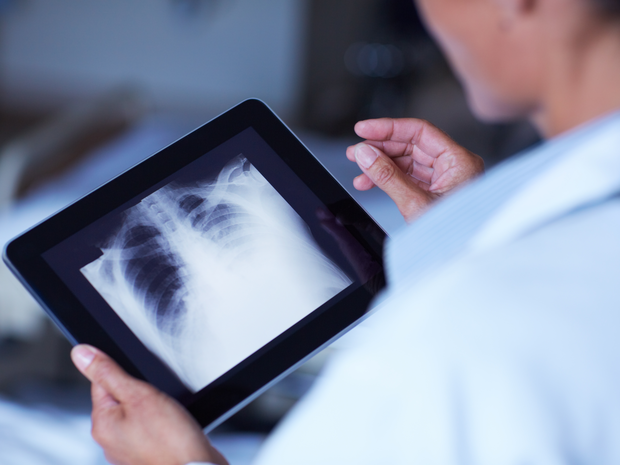
Chest X-ray/CT Scan
In any patient with CF, lung infections, inflammation, and scarring can occur early in life. These lung problems may or may not create symptoms, and may or may not show in pulmonary function testing.
- A chest x-ray allows us to see if there is any damage, to establish a baseline allowing comparison of subsequent chest x-rays, and to provide a diagnostic tool. These results also help us identify a need for inhaled medications.
- A high resolution computerized tomography (HRCT) scan of the chest helps us see if structural damage has occurred in the lungs and establish a baseline for future comparison. The HRCT is sensitive enough to find small areas of mucus plugging, inflammation and early damage in the lungs.

Pulmonary Function Tests
During each clinical visit, we’ll use a hand held device called a spirometer to measure FVC (forced vital capacity) and FEV1 (forced expiratory volume in one second). The FVC measures the total amount of air a person can breathe out forcefully after one deep breath while the FEV1 measures the amount of air forced out in the first second of the FVC. These two tests help a clinician identify any lung volume abnormalities and which therapies can help to improve them.
While this type of testing typically begins around age 6, children are often introduced to the testing equipment and the associated deep-breathing maneuvers earlier to help them prepare. Results factor in a child’s age, sex, height, and weight.
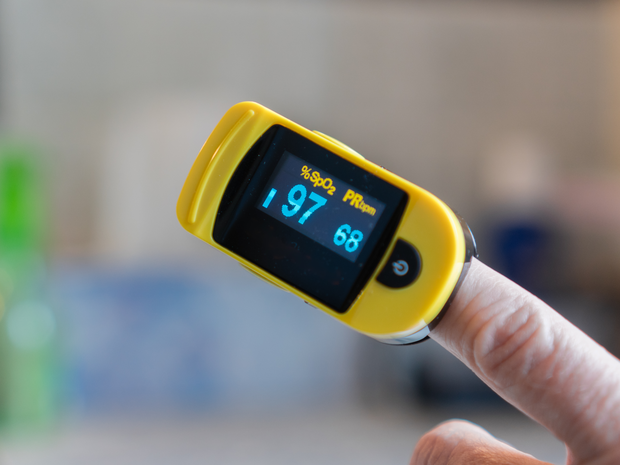
Pulse Oximetry
Pulse oximetry estimates the amount of oxygen in the blood. This measurement is taken by shining specific wave lengths of light through one side of an appendage (typically a finger) and measuring the amount of light that makes it through to the other side. A computer then calculates an estimated percentage of oxygen in the blood, usually referred to as oxygen saturation level (or “sat” for short).
A normal oxygen saturation is over 90%. When sat levels fall below 90%, your heart, lungs, and blood vessels must work much harder than usual to deliver adequate oxygen to your body. Over time, this extra work can cause permanent injury. Often, an inadequate oxygen saturation level is caused by a lung problem. If lung tissue is damaged, inflamed, or blocked, your body cannot capture enough oxygen from the air you breathe.
We’ll check your oxygen saturation as part of each routine checkup at the CF clinic.

Sputum Samples
Sputum is a thick fluid made in the lungs and in the airways leading to the lungs. A sputum culture is a test to find germs (such as bacteria or a fungus) that can cause an infection.
At each clinic visit, our respiratory therapist will obtain a sputum sample or a throat culture to test for respiratory infection. You will be asked to cough into a sterile cup for the sputum sample. If you are not able to cough up a sample, we will swab the back of your throat with a soft, flexible cotton swab. If there is a new infection present, you will be contacted by the doctor or nurse coordinator and prescribed antibiotics.