Population Management, Past and Future
I am privileged to work with many outstanding physician leaders, one of whom is Dr. Kurt Seppi, our executive medical director. Dr. Seppi’s responsibilities include oversight of all of St. Luke’s clinics.
Dr. Seppi’s work has been focused on our transformation to accountable care, the achievement of the Triple Aim, and the transformation of our clinical care model. Central to this is the development of capabilities and competencies to manage the health of populations.
Population health management was the theme for St. Luke’s Health System’s Annual Summit in February and my Spring Visits held during the past few weeks across our System. In today’s guest blog, Dr. Seppi does a great job of connecting the dots while explaining the objectives and approach to achieving accountable care for the populations we are privileged to serve.
I was raised in Lava Hot Springs, a small town in eastern Idaho. My father’s dentistry practice was located in the only hospital in the area. Its medical staff consisted of one general practitioner.
This physician, Dr. Leo Burkett, was the sole provider for the entire area. He truly cared for the entire regional population from cradle to grave, delivering babies, providing pediatric and general medical care, and performing surgery. I have surgical scars from a hernia repair and an open reduction of a clavicular fracture as proof of his abilities.
He was a central figure in the fabric of the community and a constant on the sidelines of almost every high school sporting event. His dedication to and compassion for the people in that region was an inspiration to all and the major reason I pursued a career in medicine, and specifically, family practice.
Medicine has gotten more complicated since Dr. Burkett’s time. The advances in medicine associated with sub-specialization and improvements in technology and innovation have made a tremendous impact in countless lives, but the price of this success has included increasing complexity of the system, fragmentation and silos of care, and exorbitant increases in cost that are becoming unsustainable. We must address these problems collaboratively without going back the days of Dr. Burkett.

I have been witness to these challenges, which are generally system and process problems, during my 28 years of practice. Patients need providers and they need hospitals, but most importantly, they need physicians and hospitals to all work together.
I have another perspective that I bring to my role, because in addition to practicing in Boise for four years and Twin Falls for 24 years, I also have had the opportunity to serve as a board member for a major health insurance company for 17 years.
My initial skepticism was replaced over time with an understanding of the financing challenges of health care. To a great extent, providers and hospitals have abdicated responsibility or accountability for the cost of care delivery and have left that up to the insurance industry.
But since the insurance industry is not capable of providing care or responsible for the provision of care, it has limited ability to address the cost of care, except through utilization management techniques. This has caused adversarial relationships with patients and providers.
As a consequence of my experience working with patients, providers, hospitals, and payers, I have come to the realization that transformation of health care will require collaboration and partnerships with all of these major stakeholders and others.
At St. Luke’s, our mission statement, “to improve the health of people in our region,” defines why we exist. And our vision statement makes it clear that St. Luke’s is committed to transforming health care by partnering with physicians and other providers to deliver integrated and seamless care across all care sites.
In addition to working with major stakeholders, our strategy for transformation is to provide accountable care for a defined population of patients where providers:
- Take responsibility for a defined population.
- Coordinate care across all care settings.
- Are held to benchmarks of quality and cost.
No matter how successful we are at prevention and health maintenance, people still will become “patients,” and then we need to provide care that is safe, timely, effective, efficient, equitable and patient-centered.
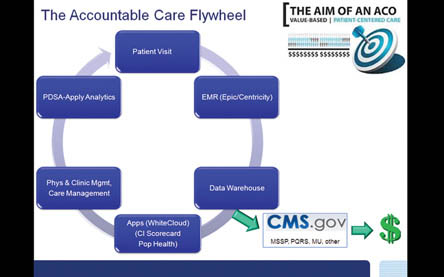
This “Accountable Care Flywheel” shows how we are addressing our population management criteria, detailed in the report posted below in the blog, and the sequence in which they will be used to drive process improvement:
St. Luke’s has participated in the Medical Shared Savings Program as the only Idaho-based ACO since January 2013.
The program requires a minimum level of performance on quality and service for the ACO to quality for any potential savings on the care of a defined population of Medicare beneficiaries.
St Luke’s Clinic had 24,865 Medicare beneficiaries that were identified as potential participants in the program, with 24,234 agreeing to participate.
During the first year of the ACO, we successfully reported on the 33 measures required for all beneficiaries within the relatively short time frame allotted. In doing so, St Luke’s has qualified to receive the entire amount of our share of savings that are realized compared with benchmark data.
This is a major accomplishment, made possible by the work done on implementation of electronic health records, our enterprise data warehouse, and monitoring tools including our clinical integration scorecard and population management modules as illustrated in the flywheel.
In the second and third years of the program, performance metrics benchmarked against other ACOs around the country will become more influential in determining the amount of shared savings we can receive.
Due to our analytic tools and capabilities, we have been able to measure our performance on quality and service measures required by the Centers for Medicare & Medicaid Services, even though we will not be held to those measures until the last two years of the program.
Based on our findings, we would qualify for 90 percent and 88 percent of shared savings in years 2014 and 2015, respectively, if we were reimbursed on today’s performance.
Just being able to measure our performance is a differentiating factor that sets us apart from many of the other ACOs around the nation. This speaks volumes about our ability to not only measure our performance, which is no small task, but also to the quality of care we are providing, which should only get better as we implement standardized work flows and process improvement initiatives.
Click here for a graphical representation of how we have performed.
In closing, I would like to recognize the fantastic work done by our providers, administration, and staff members over the past few years. This has been an unprecedented time of change in health care, and the pace of change will likely accelerate.
Such rapid change can be accompanied by feelings of frustration, uncertainty and loss of control, but we should not lose sight of the progress we have made in a few short years by working together.
Improving the health of all people in our region is a worthy goal. We are privileged to play a central part in shaping the future of health care as we choose to lead this transformation. I would like to think that Dr. Burkett would approve of our commitment to our community and what we are trying to accomplish.
About The Author

David C. Pate, M.D., J.D., previously served as president and CEO of St. Luke's Health System, based in Boise, Idaho. Dr. Pate joined the System in 2009 and retired in 2020. He received his medical degree from Baylor College of Medicine in Houston and his law degree from the University of Houston Law Center.
