Alpha-1 Antitrypsin Deficiency Genetic Testing
Overview
Alpha-1 antitrypsin (AAT) is a protein normally found in the lungs and the bloodstream. It helps protect the lungs from diseases such as emphysema and chronic obstructive pulmonary disease (COPD). Some people do not make enough of this protein or they make an abnormal type of AAT, either of which can cause AAT deficiency. These people are more likely to have lung diseases and will get them at a younger-than-normal age (30 to 40 years old). Some types of abnormal AAT can also damage the liver. AAT deficiency is a rare disorder and is the only known genetic (inherited) factor that increases your chances for developing emphysema.
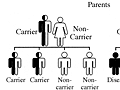
Alpha-1 antitrypsin deficiency is caused by a change, or mutation, in the gene that tells the body how to make alpha-1 antitrypsin. There are many kinds of possible changes in this gene, but only a few cause problems. To have this condition, you have to get the changed gene from both parents.
If you receive only one changed gene, you do not have the disease but are a carrier. The good copy of the gene you received from your other parent is enough to tell your body how to properly make alpha-1 antitrypsin. Some people who carry the changed gene may have very mild symptoms of the deficiency.
Treatment for alpha-1 antitrypsin deficiency involves avoiding substances—especially cigarette smoke—that could harm your lungs. Also try to avoid dust and workplace chemicals. You also may want to avoid alcohol because of the risk of liver damage. Exercise can improve your stamina and overall health. You may also need medicines and other treatments to help you breathe easier and stay as healthy and strong as you can.
The only treatment available for the lack of the protein is plasma containing alpha-1 antitrypsin. This is usually given only to people who have very low levels of AAT in their blood. It is not clear that this treatment is any better than avoiding smoke and other lung-damaging chemicals. The plasma is made from the blood of many donors and is treated to reduce the chance of spreading an infectious disease. You receive the plasma through an I.V., usually every 3 to 4 weeks for life.
About the Test
A blood test can measure the amount of alpha-1 antitrypsin (AAT) in your blood. You may have AAT deficiency if your levels are low or if the blood test is not able to find any AAT in your blood. If your AAT level is lower than normal, the blood sample can be tested to look for abnormal types of alpha-1 antitrypsin. People who carry the changed gene may be more at risk for symptoms if they have certain types of alpha-1 antitrypsin.
Normal alpha-1 antitrypsin levels are 100–200 mg/dL or 1.0–2.0 g/L.footnote 1
Although this blood test is highly reliable, no test is 100% accurate. This test cannot predict when—or whether—you will develop symptoms or how severe they will be.
Deciding About Testing
The decision to have the test is personal. You may have emotional, financial, and family reasons for taking or not taking the test.
You may choose to have the test because:
- You have unexplained lung problems and want to know whether you have this condition.
- You have been diagnosed with emphysema or COPD and want to find out if you have AAT deficiency.
- Other people in your family have AAT deficiency.
- Other people in your family have unexplained lung disease or liver disease.
- You want to take steps to protect your health if you find out you have the condition.
- You would be relieved to know that you do not have the changed gene.
- You would change your decision about having children because of test results.
- Your insurance would pay for the test.
You may decide not to be tested because:
- You do not have symptoms of lung disease.
- No one in your family has AAT deficiency or lung or liver disease.
- You would be worried if you knew that you might get lung or liver disease some day.
- You do not smoke and you already are taking good care of yourself. You think there is nothing more you could do to prevent or delay the disease.
- The test cannot predict whether you will ever have symptoms of this condition.
- You do not have insurance or your insurance would not pay for the test.
- You are worried that the test results might cause problems for you at work or make it hard for you to get health insurance. It's important to know that a law in the United States, called the Genetic Information Nondiscrimination Act of 2008 (GINA), protects people who have genetic differences that may affect their health. GINA prevents employers and health insurance companies from using genetic information about people to affect decisions. This law does not cover life insurance, disability insurance, or long-term care insurance. And it doesn't protect people who work for companies with fewer than 15 employees.
Learn more
Genetic Counseling
The results of genetic testing can affect your life. It may be a good idea to get genetic counseling before deciding to have testing. Genetic counselors can explain the pros and cons of testing, but you make the decision about whether to have the test. A genetic counselor can help you make well-informed decisions. Genetic counseling can help you and your family:
- Understand medical facts about a disease and what you may be able to do to manage it.
- Understand how your family history contributes to the development of a disease.
- Explain the results of a genetic test.
- Help you find resources, including getting referrals to specialists or finding local support groups.
Genetic counselors have specialized training in medical genetics and counseling. They are sensitive to the physical and emotional aspects of these decisions. Your privacy and confidentiality are carefully protected.
Learn more
References
Citations
Credits
Current as of: April 2, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.
Current as of: April 2, 2023
Author: Healthwise Staff
Clinical Review Board
All Healthwise education is reviewed by a team that includes physicians, nurses, advanced practitioners, registered dieticians, and other healthcare professionals.